Psychological pain
Psychological pain, mental pain, or emotional pain is an unpleasant feeling (a suffering) of a psychological, non-physical origin. A pioneer in the field of suicidology, Edwin S. Shneidman, described it as "how much you hurt as a human being. It is mental suffering; mental torment."[1] There is no shortage in the many ways psychological pain is referred to, and using a different word usually reflects an emphasis on a particular aspect of mind life. Technical terms include algopsychalia and psychalgia,[2] but it may also be called mental pain,[3][4] emotional pain,[5] psychic pain,[6][7] social pain,[8] spiritual or soul pain,[9] or suffering.[10][11] While these clearly are not equivalent terms, one systematic comparison of theories and models of psychological pain, psychic pain, emotional pain, and suffering concluded that each describe the same profoundly unpleasant feeling.[12] Psychological pain is believed to be an inescapable aspect of human existence.[13]
| Psychological pain | |
|---|---|
| Other names | Suffering, mental agony, mental pain, emotional pain, algopsychalia, psychic pain, social pain, spiritual pain, soul pain |
 | |
| Vincent van Gogh's 1890 painting Sorrowing old man ('At Eternity's Gate'), where a man weeps due to the unpleasant feelings of psychological pain. | |
| Specialty | Psychiatry, psychology |
| Medication | Antidepressant medication, Analgesic medication |
Other descriptions of psychological pain are "a wide range of subjective experiences characterized as an awareness of negative changes in the self and in its functions accompanied by negative feelings",[14] "a diffuse subjective experience ... differentiated from physical pain which is often localized and associated with noxious physical stimuli",[15] and "a lasting, unsustainable, and unpleasant feeling resulting from negative appraisal of an inability or deficiency of the self."[12]
Cause
The adjective 'psychological' is thought to encompass the functions of beliefs, thoughts, feelings, and behaviors,[16] which may be seen as an indication for the many sources of psychological pain. One way of grouping these different sources of pain was offered by Shneidman, who stated that psychological pain is caused by frustrated psychological needs.[1] For example, the need for love, autonomy, affiliation, and achievement, or the need to avoid harm, shame, and embarrassment. Psychological needs were originally described by Henry Murray in 1938 as needs that motivate human behavior.[17] Shneidman maintained that people rate the importance of each need differently, which explains why people's level of psychological pain differs when confronted with the same frustrated need. This needs perspective coincides with Patrick David Wall's description of physical pain that says that physical pain indicates a need state much more than a sensory experience.[18]
In the fields of social psychology and personality psychology, the term social pain is used to denote psychological pain caused by harm or threat to social connection; bereavement, embarrassment, shame and hurt feelings are subtypes of social pain.[19] From an evolutionary perspective, psychological pain forces the assessment of actual or potential social problems that might reduce the individual's fitness for survival.[20] The way we display our psychological pain socially (for example, crying, shouting, moaning) serves the purpose of indicating that we are in need.
Emotional agony in borderline personality disorder
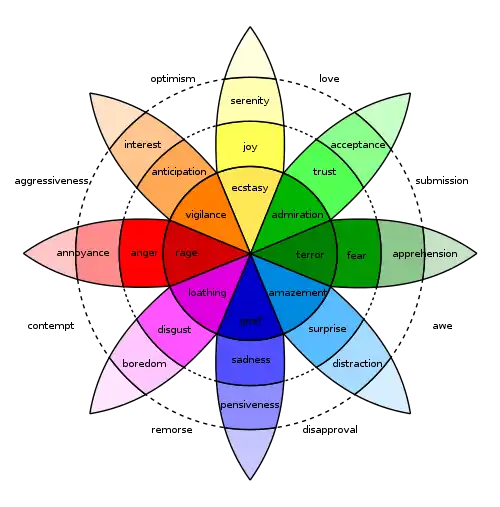
Borderline personality disorder (BPD) has long been believed to be the one psychiatric disorder that produced the most intense emotional pain, agony, and distress in those who suffer with this condition. Studies have shown that borderline patients experience chronic and significant emotional suffering and mental agony.[21][22] Borderline patients may feel overwhelmed by negative emotions, experiencing intense grief instead of sadness, shame and humiliation instead of mild embarrassment, rage instead of annoyance, and panic instead of nervousness.[23] People with BPD are especially sensitive to feelings of rejection, isolation and perceived failure.[24] Both clinicians and laymen alike have witnessed the desperate attempts to escape these subjective inner experiences of these patients. Borderline patients are severely impulsive and their attempts to alleviate the agony are often very destructive or self-destructive. Suicidal ideation, suicide attempts, eating disorders (anorexia nervosa, binge eating disorder, and bulimia nervosa), self-harm (cutting, overdosing, starvation, etc.), compulsive spending, gambling, sex addiction, violent and aggressive behaviour, sexual promiscuity and deviant sexual behaviours, are desperate attempts to escape. The intrapsychic pain experienced by those diagnosed with BPD has been studied and compared to normal healthy controls and to others suffering from major depression, bipolar disorder, substance use disorder, schizophrenia, other personality disorders, and a range of other conditions. The excruciatingly painful inner experience of the borderline patient is both unique and perplexing. In clinical populations, the rate of suicide of patients with borderline personality disorder is estimated to be 10%, a rate far greater than that in the general population and still considerably greater than for patients with schizophrenia and bipolar disorder. However, since 60–70% of patients with borderline personality disorder make suicide attempts; suicide attempts are far more frequent than completed suicides in patients with borderline personality disorder.[25]
The intense dysphoric states which patients diagnosed with borderline personality disorder (BPD) endure on a regular basis distinguishes them from those suffering from other personality disorders, major depressive disorder, bipolar disorder, and virtually all known Axis I and Axis II conditions. In a 1998 study entitled "The Pain of Being Borderline: Dysphoric States Specific to Borderline Personality Disorder", one hundred and forty six diagnosed borderline patients took a 50-item self-report measure test. The conclusions from this study suggest "that the subjective pain of borderline patients may be both more pervasive and more multifaceted than previously recognized and that the overall “amplitude” of this pain may be a particularly good marker for the borderline diagnosis".[26]
Neural mechanisms
Research suggests that physical pain and psychological pain may share some underlying neurological mechanisms.[27][28][29][30] Brain regions that were consistently found to be implicated in both types of pain are the anterior cingulate cortex and prefrontal cortex (some subregions more than others), and may extend to other regions as well. Brain regions that were also found to be involved in psychological pain include the insular cortex, posterior cingulate cortex, thalamus, parahippocampal gyrus, basal ganglia, and cerebellum. Some advocate that, because similar brain regions are involved in both physical pain and psychological pain, we should see pain as a continuum that ranges from purely physical to purely psychological.[31] Moreover, many sources mention the fact that we use metaphors of physical pain to refer to psychological pain experiences.[8][12][32] Further connection between physical and psychological pain has been supported through proof that acetaminophen, an analgesic, can suppress activity in the anterior cingulate cortex and the insular cortex when experiencing social exclusion, the same way that it suppresses activity when experiencing physical pain.[33][34] and reduces the agitation of people with dementia.[35][36] However use of paracetamol for more general psychological pain remains disputed.[37]
Religious Perspectives
Many religious traditions, such as the Noble Eightfold Path in Buddhism, have attempted or managed to provide treatment of psychological suffering. Meditation has mental health benefits.[38][39] The most common form of meditative practice as therapy is mindfulness, but breath focused exercises are also used for dealing with the stresses and anxiety related to emotional pain, reducing physiological symptoms.
See also
References
- Shneidman ES. The Suicidal Mind. Oxford University Press; 1996. ISBN 9780195118018. Appendix A Psychological Pain Survey. p. 173.
- Psychalgia: mental distress. Merriam-Webster's Medical Dictionary. But see also psychalgia in the sense of psychogenic pain.
- Weiss E. Bodily pain and mental pain. The International Journal of Psychoanalysis. 1934;15:1–13.
- Orbach I, Mikulincer M, Gilboa-Schechtman E, Sirota P. Mental pain and its relationship to suicidality and life meaning. Suicide and Life-Threatening Behavior. 2003;33(3):231–41. doi:10.1521/suli.33.3.231.23213.
- Bolger EA. Grounded theory analysis of emotional pain. Psychotherapy Research. 1999;9(3):342–62. doi:10.1080/10503309912331332801.
- Joffe WG, Sandler J. On the concept of pain, with special reference to depression and psychogenic pain. Journal of Psychosomatic Research. 1967;11(1):69–75. doi:10.1016/0022-3999(67)90058-X.
- Shattell MM. Why does "pain management" exclude psychic pain?. Issues in Mental Health Nursing. 2009;30(5):344. doi:10.1080/01612840902844890.
- Macdonald G, Leary MR.. Why does social exclusion hurt? The relationship between social and physical pain. Psychological Bulletin. 2005 [archived 2014-03-01];131(2):202–23. doi:10.1037/0033-2909.131.2.202. PMID 15740417.
- Spiritual pain: 60,000 Google results. Soul pain: 237,000 Google results.
- Morse JM. Toward a praxis theory of suffering. Advances in Nursing Science. 2001;24(1):47–59. doi:10.1097/00012272-200109000-00007.
- Rehnsfeldt A, Eriksson K. The progression of suffering implies alleviated suffering. Scandinavian Journal of Caring Sciences. 2004;18(3):264–72. doi:10.1111/j.1471-6712.2004.00281.x.
- Meerwijk EL, Weiss SJ. Toward a unifying definition of psychological pain. Journal of Loss & Trauma. 2011;16(5):402–12. doi:10.1080/15325024.2011.572044.
- Wille RSG.. On the capacity to endure psychic pain. The Scandinavian Psychoanalytic Review. 2011;34:23–30. doi:10.1080/01062301.2011.10592880.
- Orbach I, Mikulincer M, Sirota P, Gilboa-Schechtman E. Mental pain: A multidimensional operationalization and definition. Suicide and Life-Threatening Behavior. 2003;33(3):219–30. doi:10.1521/suli.33.3.219.23219.
- Mee S, Bunney BG, Reist C, Potkin SG, Bunney WE. Psychological pain: a review of evidence. Journal of Psychiatric Research. 2006;40(8):680–90. doi:10.1016/j.jpsychires.2006.03.003.
- Covington EC. Psychogenic pain--What it means, why it does not exist, and how to diagnose it. Pain Medicine. 2000;1(4):287–94. doi:10.1046/j.1526-4637.2000.00049.x.
- Murray HA (2008). Explorations in personality (70 ed.). New York, NY: Oxford University Press. ISBN 978-0-19-530506-7.
- Wall PD.. On the relation of injury to pain. Pain. 1979;6:253–64. doi:10.1016/0304-3959(79)90047-2.
- MacDonald, Geoff (2009). "Social Pain and Hurt Feelings" (PDF). In Corr, Philip J.; Matthews, Gerald (eds.). Cambridge Handbook of Personality Psychology. Cambridge UK: Cambridge University Press. ISBN 9780521680516.
- Thornhill R, Wilmsen Thornhill N. (1989). "The Evolution of Psychological Pain". In Bell, RW; Bell, NJ (eds.). Sociobiology and the Social Sciences. Lubbock, Texas: Texas Tech University Press. ISBN 978-0-89672-161-6.
- Fertuck, EA.; Jekal, A.; Song, I.; Wyman, B.; Morris, MC.; Wilson, ST.; Brodsky, BS.; Stanley, B. (December 2009). "Enhanced 'Reading the Mind in the Eyes' in borderline personality disorder compared to healthy controls". Psychological Medicine. 39 (12): 1979–1988. doi:10.1017/S003329170900600X. PMC 3427787. PMID 19460187.
- Diagnostic and Statistical Manual of Mental Disorders (DSM-IV) (4th ed.). Washington, DC: American Psychiatric Association. 1994. ISBN 978-0-89-042061-4.
- Linehan 1993, p. 44
- Stiglmayr CE, Grathwol T, Linehan MM, Ihorst G, Fahrenberg J, Bohus M (May 2005). "Aversive tension in patients with borderline personality disorder: a computer-based controlled field study". Acta Psychiatr Scand. 111 (5): 372–9. doi:10.1111/j.1600-0447.2004.00466.x. PMID 15819731. S2CID 30951552.
- Oldham, JM (2006). "Borderline Personality Disorder and Suicidality". The American Journal of Psychiatry. 163 (1): 20–26. doi:10.1176/appi.ajp.163.1.20. PMID 16390884.
- Zanarini, MC; Gunderson, JG; Frankenburg, FR; DeLuca, CJ; Hennen, J; Khera, GS (1998). "The Pain of Being Borderline: Dysphoric States Specific to Borderline Personality Disorder". Harvard Review of Psychiatry. 6 (4): 201–207. doi:10.3109/10673229809000330. PMID 10370445. S2CID 10093822.
- Eisenberger, NI (2012). "The neural bases of social pain: Evidence for shared representations with physical pain". Psychosomatic Medicine. 74 (2): 126–35. doi:10.1097/PSY.0b013e3182464dd1. PMC 3273616. PMID 22286852.
- Mee, S, Bunney, BG, Reist, C, Potkin, SG, & Bunney, WE.. Psychological pain: a review of evidence. Journal of Psychiatric Research. 2006;40(8):680–90. doi:10.1016/j.jpsychires.2006.03.003.
- Eisenberger, Naomi I.; Lieberman, Matthew D. (Jul 2004). "Why rejection hurts: a common neural alarm system for physical and social pain". Trends Cogn Sci. 8 (7): 294–300. doi:10.1016/j.tics.2004.05.010. PMID 15242688. S2CID 15893740.
- Meerwijk, EL, Ford, JM, & Weiss, SJ.. Brain regions associated with psychological pain: implications for a neural network and its relationship to physical pain. Brain Imaging Behav. 2012. doi:10.1007/s11682-012-9179-y.
- Biro D.. Is there such a thing as psychological pain? and why It matters. Culture, Medicine and Psychiatry. 2010;34(4):658–67. doi:10.1007/s11013-010-9190-y.
- Flaskerud JH.. Heartbreak and physical pain linked in brain. Issues in Mental Health Nursing. 2011;32:789–91. doi:10.3109/01612840.2011.583714.
- Dewall, C. N., Macdonald, G., Webster, G. D., Masten, C. L., Baumeister, R. F., Powell, C., . . . Eisenberger, N. I. (2010). Acetaminophen Reduces Social Pain: Behavioral and Neural Evidence. Psychological Science, 21(7), 931-937. doi:10.1177/0956797610374741
- Randles, Daniel; Heine, Steven J.; Santos, Nathan (2013). "The Common Pain of Surrealism and Death". Psychological Science. 24 (6): 966–973. doi:10.1177/0956797612464786. PMID 23579320. S2CID 2890442.
- Husebo, B. S.; Ballard, C.; Sandvik, R.; Nilsen, O. B.; Aarsland, D. (2011). "Efficacy of treating pain to reduce behavioural disturbances in residents of nursing homes with dementia: cluster randomised clinical trial". BMJ. 343: d4065. doi:10.1136/bmj.d4065. PMC 3137923. PMID 21765198.
- "Reducing agitation through pain relief - Living with dementia magazine October 2011 - Alzheimer's Society". alzheimers.org.uk.
- "Don't take paracetamol for painful emotions". www.nhs.uk. 2013-04-22.
- "Meditation changes the brain". www.nhs.uk. 2010-08-17.
- "Mindfulness Meditation". Harvard Gazette. Retrieved 2018-05-01.