Hypercalcaemia
Hypercalcaemia, also spelled hypercalcemia, is a high calcium (Ca2+) level in the blood serum.[1][3] The normal range is 2.1–2.6 mmol/L (8.8–10.7 mg/dL, 4.3–5.2 mEq/L), with levels greater than 2.6 mmol/L defined as hypercalcemia.[1][2][4] Those with a mild increase that has developed slowly typically have no symptoms.[1] In those with greater levels or rapid onset, symptoms may include abdominal pain, bone pain, confusion, depression, weakness, kidney stones or an abnormal heart rhythm including cardiac arrest.[1][2]
| Hypercalcaemia | |
|---|---|
| Other names | Hypercalcemia |
 | |
| Calcium within the periodic table | |
| Specialty | Endocrinology |
| Symptoms | Abdominal pain, bone pain, confusion, depression, weakness[1][2] |
| Complications | Kidney stones, abnormal heart rhythm, cardiac arrest[1][2] |
| Causes | Primary hyperparathyroidism, cancer, sarcoidosis, tuberculosis, Paget disease, multiple endocrine neoplasia, vitamin D toxicity[1][3] |
| Diagnostic method | Blood serum level > 2.6 mmol/l (corrected calcium or ionized calcium)[1][2] |
| Treatment | Underlying cause, intravenous fluids, furosemide, calcitonin, pamidronate, hemodialysis[1][2] |
| Frequency | 4 per 1,000[1] |
Most cases are due to primary hyperparathyroidism or cancer.[1] Other causes include sarcoidosis, tuberculosis, Paget disease, multiple endocrine neoplasia (MEN), vitamin D toxicity, familial hypocalciuric hypercalcaemia and certain medications such as lithium and hydrochlorothiazide.[1][2][3] Diagnosis should generally include either a corrected calcium or ionized calcium level and be confirmed after a week.[1] Specific changes, such as a shortened QT interval and prolonged PR interval, may be seen on an electrocardiogram (ECG).[2]
Treatment may include intravenous fluids, furosemide, calcitonin or pamidronate in addition to treating the underlying cause.[1][2] The evidence for furosemide use, however, is poor.[1] In those with very high levels, hospitalization may be required.[1] Haemodialysis may be used in those who do not respond to other treatments.[1] In those with vitamin D toxicity, steroids may be useful.[1] Hypercalcemia is relatively common.[1] Primary hyperparathyroidism occurs in 1–7 per 1,000 people, and hypercalcaemia occurs in about 2.7% of those with cancer.[1]
Signs and symptoms
| Stones | Kidney or biliary |
| Bones | Bone pain |
| Groans | Abdominal discomfort |
| Moans | Complaints of non-specific symptoms |
| Thrones | Constipation and frequent urination |
| Muscle tone | Muscle weakness, decreased reflexes |
| Psychiatric overtones | Depression, anxiety, cognitive dysfunction |
The neuromuscular symptoms of hypercalcaemia are caused by a negative bathmotropic effect due to the increased interaction of calcium with sodium channels. Since calcium blocks sodium channels and inhibits depolarization of nerve and muscle fibers, increased calcium raises the threshold for depolarization.[5] This results in diminished deep tendon reflexes (hyporeflexia), and skeletal muscle weakness.[6]
Other symptoms include cardiac arrhythmias (especially in those taking digoxin), fatigue, nausea, vomiting (emesis), loss of appetite, abdominal pain, & paralytic ileus. If kidney impairment occurs as a result, manifestations can include increased urination, urination at night, and increased thirst.[6] Psychiatric manifestation can include emotional instability, confusion, delirium, psychosis, and stupor.[6] Calcium deposits known as limbus sign may be visible in the eyes.
Symptoms are more common at high calcium blood values (12.0 mg/dl or 3 mmol/l).[6] Severe hypercalcaemia (above 15–16 mg/dl or 3.75–4 mmol/l) is considered a medical emergency: at these levels, coma and cardiac arrest can result. The high levels of calcium ions decrease the neuron membrane permeability to sodium ions, thus decreasing excitability, which leads to hypotonicity of smooth and striated muscle. This explains the fatigue, muscle weakness, low tone and sluggish reflexes in muscle groups. The sluggish nerves also explain drowsiness, confusion, hallucinations, stupor or coma. In the gut this causes constipation. Hypocalcaemia causes the opposite by the same mechanism.
Hypercalcaemic crisis
A hypercalcaemic crisis is an emergency situation with a severe hypercalcaemia, generally above approximately 14 mg/dL (or 3.5 mmol/l).[7]
The main symptoms of a hypercalcaemic crisis are oliguria or anuria, as well as somnolence or coma.[8] After recognition, primary hyperparathyroidism should be proved or excluded.[8]
In extreme cases of primary hyperparathyroidism, removal of the parathyroid gland after surgical neck exploration is the only way to avoid death.[8] The diagnostic program should be performed within hours, in parallel with measures to lower serum calcium.[8] Treatment of choice for acutely lowering calcium is extensive hydration and calcitonin, as well as bisphosphonates (which have effect on calcium levels after one or two days).[9]
Causes
Primary hyperparathyroidism and malignancy account for about 90% of cases of hypercalcaemia.[10][11]
Parathyroid function
- Primary hyperparathyroidism
- Solitary parathyroid adenoma
- Primary parathyroid hyperplasia
- Parathyroid carcinoma
- Multiple endocrine neoplasia (MEN1 & MEN2A)
- Familial isolated hyperparathyroidism[12]
- Lithium use
- Familial hypocalciuric hypercalcemia/familial benign hypercalcemia[13][14][15]
Cancer
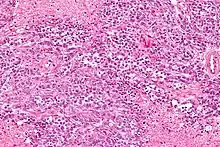
- Solid tumour with metastasis (e.g. breast cancer or classically squamous cell carcinoma, which can be PTHrP-mediated)
- Solid tumour with humoral mediation of hypercalcaemia (e.g. lung cancer, most commonly non-small cell lung cancer[16] or kidney cancer, phaeochromocytoma)
- Haematologic cancers (multiple myeloma, lymphoma, leukaemia)
- Ovarian small cell carcinoma of the hypercalcemic type
Vitamin-D disorders
- Hypervitaminosis D (vitamin D intoxication)
- Elevated 1,25(OH)2D (see calcitriol under Vitamin D) levels (e.g. sarcoidosis and other granulomatous diseases such as tuberculosis, berylliosis, histoplasmosis, Crohn's disease, and granulomatosis with polyangiitis)
- Idiopathic hypercalcaemia of infancy[17]
- Rebound hypercalcaemia after rhabdomyolysis
High bone-turnover
- Hyperthyroidism
- Multiple myeloma
- Prolonged immobilization
- Paget's disease
- Thiazide use
- Vitamin A intoxication
Kidney failure
- Tertiary hyperparathyroidism
- Aluminium intoxication
- Milk-alkali syndrome
Diagnosis
Diagnosis should generally include either a corrected calcium or ionized calcium level and be confirmed after a week.[1] There is, however, controversy around the usefulness of corrected calcium as it may be no better than total calcium.[18]
The normal range is 2.1–2.6 mmol/L (8.8–10.7 mg/dL, 4.3–5.2 mEq/L), with levels greater than 2.6 mmol/L defined as hypercalcaemia.[1][2][4] Moderate hypercalcaemia is a level of 2.88–3.5 mmol/L (11.5–14 mg/dL) while severe hypercalcaemia is > 3.5 mmol/L (>14 mg/dL).[19]
ECG

Abnormal heart rhythms can also result, and ECG findings of a short QT interval[20] suggest hypercalcaemia. Significant hypercalcaemia can cause ECG changes mimicking an acute myocardial infarction.[21] Hypercalcaemia has also been known to cause an ECG finding mimicking hypothermia, known as an Osborn wave.[22]
Treatments
The goal of therapy is to treat the hypercalcaemia first and subsequently effort is directed to treat the underlying cause.
Fluids and diuretics
Initial therapy:
- hydration, increasing salt intake, and forced diuresis.
- hydration is needed because many patients are dehydrated due to vomiting or kidney defects in concentrating urine.
- increased salt intake also can increase body fluid volume as well as increasing urine sodium excretion, which further increases urinary calcium excretion.
- after rehydration, a loop diuretic such as furosemide can be given to permit continued large volume intravenous salt and water replacement while minimizing the risk of blood volume overload and pulmonary oedema. In addition, loop diuretics tend to depress calcium reabsorption by the kidney thereby helping to lower blood calcium levels
- can usually decrease serum calcium by 1–3 mg/dL within 24 hours
- caution must be taken to prevent potassium or magnesium depletion
Bisphosphonates and calcitonin
Additional therapy:
- bisphosphonates are pyrophosphate analogues with high affinity for bone, especially areas of high bone-turnover.
- they are taken up by osteoclasts and inhibit osteoclastic bone resorption
- current available drugs include (in order of potency): (1st gen) etidronate, (2nd gen) tiludronate, IV pamidronate, alendronate (3rd gen) zoledronate and risedronate
- all people with cancer-associated hypercalcaemia should receive treatment with bisphosphonates since the 'first line' therapy (above) cannot be continued indefinitely nor is it without risk. Further, even if the 'first line' therapy has been effective, it is a virtual certainty that the hypercalcaemia will recur in the person with hypercalcaemia of malignancy. Use of bisphosphonates in such circumstances, then, becomes both therapeutic and preventative
- people in kidney failure and hypercalcaemia should have a risk-benefit analysis before being given bisphosphonates, since they are relatively contraindicated in kidney failure.
- Calcitonin blocks bone resorption and also increases urinary calcium excretion by inhibiting calcium reabsorption by the kidney
- Usually used in life-threatening hypercalcaemia along with rehydration, diuresis, and bisphosphonates
- Helps prevent recurrence of hypercalcaemia
- Dose is 4 international units per kilogram via subcutaneous or intramuscular route every 12 hours, usually not continued indefinitely due to quick onset of decreased response to calcitonin
Other therapies
- rarely used, or used in special circumstances
- plicamycin inhibits bone resorption (rarely used)
- gallium nitrate inhibits bone resorption and changes structure of bone crystals (rarely used)
- glucocorticoids increase urinary calcium excretion and decrease intestinal calcium absorption
- no effect on calcium level in normal or primary hyperparathyroidism
- effective in hypercalcaemia due to osteolytic malignancies (multiple myeloma, leukaemia, Hodgkin's lymphoma, carcinoma of the breast) due to antitumour properties
- also effective in hypervitaminosis D and sarcoidosis
- dialysis usually used in severe hypercalcaemia complicated by kidney failure. Supplemental phosphate should be monitored and added if necessary
- phosphate therapy can correct the hypophosphataemia in the face of hypercalcaemia and lower serum calcium
Other animals
Research has led to a better understanding of hypercalcemia in non-human animals. Often the causes of hypercalcemia have a correlation to the environment in which the organisms live. Hypercalcemia in house pets is typically due to disease, but other cases can be due to accidental ingestion of plants or chemicals in the home.[23] Outdoor animals commonly develop hypercalcemia through vitamin D toxicity from wild plants within their environments.[24]
Household pets
Household pets such as dogs and cats are found to develop hypercalcemia. It is less common in cats, and many feline cases are idiopathic.[23] In dogs, lymphosarcoma, Addison’s disease, primary hyperparathyroidism, and chronic kidney failure are the main causes of hypercalcemia, but there are also environmental causes usually unique to indoor pets.[23] Ingestion of small amounts of calcipotriene found in psoriasis cream can be fatal to a pet.[25] Calcipotriene causes a rapid rise in calcium ion levels.[25] Calcium ion levels can remain high for weeks if untreated and lead to an array of medical issues.[25] There are also cases of hypercalcemia reported due to dogs ingesting rodenticides containing a chemical similar to calcipotriene found in psoriasis cream.[25] Additionally, ingestion of household plants is a cause of hypercalcemia. Plants such as Cestrum diurnum, and Solanum malacoxylon contain ergocalciferol or cholecalciferol which cause the onset of hypercalcemia.[23] Consuming small amounts of these plants can be fatal to pets. Observable symptoms may develop such as polydipsia, polyuria, extreme fatigue, or constipation.[23]
Outdoor animals

In certain outdoor environments, animals such as horses, pigs, cattle, and sheep experience hypercalcemia commonly. In southern Brazil and Mattewara India, approximately 17 percent of sheep are affected, with 60 percent of these cases being fatal.[24] Many cases are also documented in Argentina, Papua-New Guinea, Jamaica, Hawaii, and Bavaria.[24] These cases of hypercalcemeia are usually caused by ingesting Trisetum flavescens before it has dried out.[24] Once Trisetum flavescens is dried out, the toxicity of it is diminished.[24] Other plants causing hypercalcemia are Cestrum diurnum, Nierembergia veitchii, Solanum esuriale, Solanum torvum, and Solanum malacoxylon.[24] These plants contain calcitriol or similar substances that cause rises in calcium ion levels.[24] Hypercalcemia is most common in grazing lands at altitudes above 1500 meters where growth of plants like Trisetum flavescens is favorable.[24] Even if small amounts are ingested over long periods of time, the prolonged high levels of calcium ions have large negative effects on the animals.[24] The issues these animals experience are muscle weakness, and calcification of blood vessels, heart valves, liver, kidneys, and other soft tissues, which eventually can lead to death.[24]
See also
- Calcium metabolism
- Dent's disease
- Electrolyte disturbance
- Disorders of calcium metabolism
References
- Minisola, S; Pepe, J; Piemonte, S; Cipriani, C (2015). "The diagnosis and management of hypercalcaemia". BMJ. 350: h2723. doi:10.1136/bmj.h2723. PMID 26037642. S2CID 28462200.
- Soar, Jasmeet; Perkins, Gavin D; Abbas, Gamal; Alfonzo, Annette; Barelli, Alessandro; Bierens, Joost J.L.M; Brugger, Hermann; Deakin, Charles D; Dunning, Joel; Georgiou, Marios; Handley, Anthony J; Lockey, David J; Paal, Peter; Sandroni, Claudio; Thies, Karl-Christian; Zideman, David A; Nolan, Jerry P (2010). "European Resuscitation Council Guidelines for Resuscitation 2010 Section 8. Cardiac arrest in special circumstances: Electrolyte abnormalities, poisoning, drowning, accidental hypothermia, hyperthermia, asthma, anaphylaxis, cardiac surgery, trauma, pregnancy, electrocution". Resuscitation. 81 (10): 1400–33. doi:10.1016/j.resuscitation.2010.08.015. PMID 20956045.
- "Hypercalcemia - National Library of Medicine". PubMed Health. Archived from the original on 8 September 2017. Retrieved 27 September 2016.
- "Appendix 1: Conversion of SI Units to Standard Units". Principles and Practice of Geriatric Medicine. 2. 2005. i–ii. doi:10.1002/047009057X.app01. ISBN 978-0-470-09057-2.
- Armstrong, C. M; Cota, G (1999). "Calcium block of Na+ channels and its effect on closing rate". Proceedings of the National Academy of Sciences. 96 (7): 4154–7. Bibcode:1999PNAS...96.4154A. doi:10.1073/pnas.96.7.4154. PMC 22436. PMID 10097179.
- "Hypercalcemia". Merck Manual. Archived from the original on July 13, 2017. Retrieved June 10, 2017.
- Hypercalcemia in Emergency Medicine Archived 2011-04-25 at the Wayback Machine at Medscape. Author: Robin R Hemphill. Chief Editor: Erik D Schraga. Retrieved April 2011
- Ziegler R (February 2001). "Hypercalcemic crisis". J. Am. Soc. Nephrol. 12 Suppl 17: S3–9. PMID 11251025.
- Page 394 Archived 2017-09-08 at the Wayback Machine in: Roenn, Jamie H. Von; Ann Berger; Shuster, John W. (2007). Principles and practice of palliative care and supportive oncology. Hagerstwon, MD: Lippincott Williams & Wilkins. ISBN 978-0-7817-9595-1.
- Table 20-4 in: Mitchell, Richard Sheppard; Kumar, Vinay; Abbas, Abul K.; Fausto, Nelson (2007). Robbins Basic Pathology (8th ed.). Philadelphia: Saunders. ISBN 978-1-4160-2973-1.
- Tierney, Lawrence M.; McPhee, Stephen J.; Papadakis, Maxine A. (2006). Current Medical Diagnosis and Treatment 2007 (Current Medical Diagnosis and Treatment). McGraw-Hill Professional. p. 901. ISBN 978-0-07-147247-0.
- Online Mendelian Inheritance in Man (OMIM): 146200
- Online Mendelian Inheritance in Man (OMIM): 145980
- Online Mendelian Inheritance in Man (OMIM): 145981
- Online Mendelian Inheritance in Man (OMIM): 600740
- Non-Small Cell Lung Cancer~clinical at eMedicine.
- Online Mendelian Inheritance in Man (OMIM): 143880
- Thomas, Lynn K.; Othersen, Jennifer Bohnstadt (2016). Nutrition Therapy for Chronic Kidney Disease. CRC Press. p. 116. ISBN 978-1-4398-4950-7.
- Jr, Brendan C. Stack; Bodenner, Donald L. (2016). Medical and Surgical Treatment of Parathyroid Diseases: An Evidence-Based Approach. Springer. p. 99. ISBN 978-3-319-26794-4.
- "Archived copy". Archived from the original on 2014-12-16. Retrieved 2014-10-19.CS1 maint: archived copy as title (link)
- Wesson, L; Suresh, V; Parry, R (2009). "Severe hypercalcaemia mimicking acute myocardial infarction". Clinical Medicine. 9 (2): 186–7. doi:10.7861/clinmedicine.9-2-186. PMC 4952678. PMID 19435131.
- Serafi, Sami W; Vliek, Crystal; Taremi, Mahnaz (2012). "Osborn waves in a hypothermic patient". Journal of Community Hospital Internal Medicine Perspectives. 1 (4): 10742. doi:10.3402/jchimp.v1i4.10742. PMC 3714046. PMID 23882340.
- Hypercalcemia in Dogs and Cats Archived 2014-07-28 at the Wayback Machine Peterson DVM, DACVIM. M. E., July 2013. Hypercalcemia in Dogs and Cats. The Merck Veternary Manual. Merck Sharp & Dohme, Whitehouse Station, NJ, USA.
- Enzootic Calcinosis Archived 2014-07-28 at the Wayback Machine Gruenberg MS, PhD, DECAR DECBHM. W.G., April 2014. Enzootic Calcinosis. The Merck Veternary Manual. Merck Sharp & Dohme, Whitehouse Station, NJ, USA.
- Topical Agents (Toxicity) Archived 2014-07-28 at the Wayback Machine Khan DVM, MS, PhD, DABVT, S.A., March 2012. Topical Agents (Toxicity). The Merck Veternary Manual. Merck Sharp & Dohme, Whitehouse Station, NJ, USA.
External links
| Classification | |
|---|---|
| External resources |