Ventricular aneurysm
Ventricular aneurysms are one of the many complications that may occur after a heart attack. The word aneurysm refers to a bulge or ‘pocketing’ of the wall or lining of a vessel commonly occurring in the blood vessels at the base of the septum, or within the aorta. In the heart, they usually arise from a patch of weakened tissue in a ventricular wall, which swells into a bubble filled with blood.[1] This, in turn, may block the passageways leading out of the heart, leading to severely constricted blood flow to the body. Ventricular aneurysms can be fatal. They are usually non-rupturing because they are lined by scar tissue.
| Aneurysm of heart | |
|---|---|
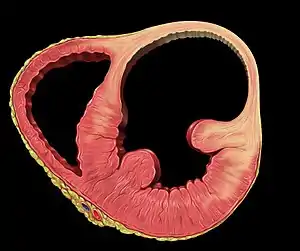 | |
| Heart left ventricular aneurysm short axis view |
A left ventricular aneurysm can be associated with ST elevation.[2]
Signs and symptoms
Ventricular aneurysms usually grow at a very slow pace, but can still pose problems. Usually, this type of aneurysm grows in the left ventricle. This bubble has the potential to block blood flow to the rest of the body, and thus limit the patient's stamina. In other cases, a similarly developed pseudoaneurysm ("false aneurysm") may burst, sometimes resulting in the death of the patient. Also, blood clots may form on the inside of ventricular aneurysms, and form embolisms. If such a clot escapes from the aneurysm, it will be moved in the circulation throughout the body. If it gets stuck inside a blood vessel, it may cause ischemia in a limb, a painful condition that can lead to reduced movement and tissue death in the limb.[1] Alternatively, if a clot blocks a vessel going to the brain, it can cause a stroke. In certain cases, ventricular aneurysms cause ventricular failure or arrythmia. At this stage, treatment is necessary.
Causes
Ventricular aneurysms are usually complications resulting from a heart attack. When the heart muscle (cardiac muscle) partially dies during a heart attack, a layer of muscle may survive, and, being severely weakened, start to become an aneurysm. Blood may flow into the surrounding dead muscle and inflate the weakened flap of muscle into a bubble. It may also be congenital.
Diagnosis
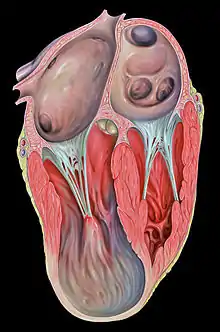

When a person visits the hospital or doctor with other symptoms, especially with a history of heart problems, they will normally be required to undergo an electrocardiogram, which monitors electrical activity within the heart and shows abnormalities when a cardiac aneurysm is present. It can also appear as a bulge on a chest x-ray, and a more accurate diagnosis will then be made using an echocardiogram, which uses ultrasound to ‘photograph’ the heart and how it functions while it beats.
Differential diagnosis
It should also not be confused with a pseudoaneurysm,[4][5] coronary artery aneurysm or a myocardial rupture (which involves a hole in the wall, not just a bulge.)
Cardiac Diverticulum
Cardiac diverticulum or ventricular diverticulum is defined as a congenital malformation of the fibrous or muscular part of the heart which is only visible during chest x-rays or during an echocardiogram reading.[6] This should not be confused with ventricular diverticulum, as the latter is a sub type derived from the latter in congenital cases. it is usually asymptomatic and is only detected using imaging. Fibrous diverticulum is characterised by a calcification if present at the tip ( apex) or a thrombi that may detaches to form an emboli. Muscular diverticulum is characterised by appendix forming at the ether of the ventricles.[7] it is a rare anomaly and can be diagnosed prenatal. Diagnosis is usually done by a chest X-ray and silhouette is viewed around the heart. Echocardiogram reading present a similar picture to ventricular aneurysms on the ST segment. Management is dependent on the situation presented and the severity of the case. Usually, surgical resection is advised but in prenatal cases, due to combination with other cardiac abnormalities, especially in latter trimesters, but pericardiocentesis is useful technique to reduce pleural effusion or/ and secondary disorders.
Treatment
Some people live with this type of aneurysm for many years without any specific treatment. Treatment is limited to surgery (ventricular reduction) for this defect of the heart. However, surgery is not required in most cases but, limiting the patient's physical activity levels to lower the risk of making the aneurysm bigger is advised. Also, ACE Inhibitors seem to prevent Left Ventricular remodeling and aneurysm formation.
Blood thinning agents may be given to help reduce the likelihood of blood thickening and clots forming, along with the use of drugs to correct the irregular rhythm of the heart (seen on the electrocardiogram)
See also
References
- "What is an Aneurysm?". www.heart.org. Retrieved 14 March 2017.
- Victor F. Froelicher; Jonathan Myers (2006). Exercise and the heart. Elsevier Health Sciences. pp. 138–. ISBN 978-1-4160-0311-3. Retrieved 10 October 2010.
- "UOTW #57 - Ultrasound of the Week". Ultrasound of the Week. 29 August 2015. Retrieved 27 May 2017.
- Zoffoli G, Mangino D, Venturini A, et al. (February 2009). "Diagnosing left ventricular aneurysm from pseudo-aneurysm: a case report and a review in literature". J Cardiothorac Surg. 4 (1): 11. doi:10.1186/1749-8090-4-11. PMC 2654444. PMID 19239694.
- Brown SL, Gropler RJ, Harris KM (May 1997). "Distinguishing left ventricular aneurysm from pseudoaneurysm. A review of the literature". Chest. 111 (5): 1403–9. doi:10.1378/chest.111.5.1403. PMID 9149600.
- Mady, Charles (1982). "Left Ventricular Diverticulum: Analysis of Two Operated Cases and Review of the Literature". Angiology. 33 (4): 280–286. doi:10.1177/000331978203300409. ISSN 0003-3197. PMID 7073021.
- Garcia Rodriguez, Raquel; Rodriguez Guedes, Azahara; Garcia Delgado, Raquel; Roldan Gutierrez, Lourdes; Medina Castellano, Margarita; Garcia Hernandez, Jose Angel (2015). "Prenatal Diagnosis of Cardiac Diverticulum with Pericardial Effusion in the First Trimester of Pregnancy with Resolution after Early Pericardiocentesis". Case Reports in Obstetrics and Gynecology. 2015: 1–11. doi:10.1155/2015/154690. ISSN 2090-6684. PMID 26558121.
Further reading
- Graber, J.D.; Oakley, C.M.; Pickering, B.N.; Goodwin, J.F.; Raphael, M.J.; Steiner, R.E. (1972). "Ventricular aneurysm. An appraisal of diagnosis and surgical treatment". British Heart Journal. PubMed. 34 (8): 831–838. doi:10.1136/hrt.34.8.831. PMC 486989. PMID 5070115.
- Alenghat, FJ; Couper, GC; Givertz, MM (2013). "Giant left ventricular aneurysm as a late complication of inferior myocardial infarction". European Heart Journal. 24 (5): 344. doi:10.1093/eurheartj/ehs357. PMID 23095983.